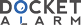`article which permits unrestricted noncommercial use, provided the original work is properly cited.
`Therapeutics and Clinical Risk Management 2009:5 375–384
`Therapeutics and Clinical Risk Management
`375
`R e v i e w
`Dovepress
`open access to scientific and medical research
`Open Access Full T ext Article
`submit your manuscript | www.dovepress.com
`Dovepress
`Casopitant: a novel NK1-receptor antagonist
`in the prevention of chemotherapy-induced
`nausea and vomiting
`Christina Ruhlmann
`Jørn Herrstedt
`Odense University Hospital,
`Department of Oncology, Odense,
`Denmark
`Correspondence: Christina Ruhlmann
`Odense University Hospital, Department
`of Oncology, Sdr. Boulevard 29, DK-5000
`Odense C, Denmark
`T el +45 6541 3834
`email christina.ruhlmann@ouh.
`regionsyd
`danmark.dk
`Abstract: Chemotherapy-induced nausea and vomiting (CINV) are among the most feared
`and distressing symptoms experienced by patients with cancer. The knowledge of the patho-
`genesis and neuropharmacology of CINV has expanded enormously over the last decades, the
`most significant discoveries being the role of 5-hydroxytryptamine (5-HT)
`3- and neurokinin
`(NK)1 receptors in the emetic reflex arch. This has led to the development of two new classes
`of antiemetics acting as highly selective antagonists at one of these receptors. These drugs
`have had a huge impact in the protection from chemotherapy-induced vomiting, whereas the
`effect on nausea seems to be limited. The first NK
`1 receptor antagonist, aprepitant, became
`clinically available in 2003, and casopitant, the second in this class of antiemetics, has now
`completed phase III trials. This review delineates the properties and clinical use of casopitant
`in the prevention of CINV.
`Keywords: casopitant, GW679769, NK
`1 receptor antagonist, chemotherapy, emesis
`Introduction
`Historically, chemotherapy-induced nausea and vomiting (CINV) are among the most
`feared and distressing symptoms experienced by patients with cancer.1 Patients’ ranking
`of side effects have changed over time. In a work by Coates and colleagues in 1983,
`patients receiving cancer chemotherapy reported vomiting and nausea as the two most
`severe side effects.
`1 In another work ten years later, the same group found that patients
`experienced nausea as the most severe side effect of chemotherapy, and vomiting was
`now ranked fifth.
`2 With the introduction of high-dose metoclopramide in 1981 the
`antiemetic outcome markedly changed, providing significant reduction in cisplatin-
`induced emesis.
`3 In the 1980s a new class of antiemetic agents, the 5-hydroxytryptamine
`(5-HT)3 receptor antagonists, were developed and became clinically available in the
`early 1990s. This further improved protection from emesis, and the efficacy was
`potentiated by addition of dexamethasone.
`4 Patients perception of side-effects in 1993
`emphasises, that the 5-HT 3-receptor antagonists are more preventive of vomiting
`than nausea, and in particular management of delayed nausea and vomiting remains
`a challenge.
`5 The latest approach towards elimination of CINV was made with the
`appearance of the neurokinin (NK)1 receptor antagonists. When added to the standard
`antiemetic regimen until 2004 (a 5-HT3-receptor antagonist and a corticosteroid), the
`NK1 receptor antagonist, aprepitant, significantly improved the percentage of patients
`with complete response (CR), defined as no emetic episodes and no rescue therapy on
`days 1 to 5 after the initiation of chemotherapy. Even a significant reduction in delayed
`emesis was demonstrated.
`6–9 In 2003, the first NK 1 receptor antagonist, aprepitant,
`HELSINN EXHIBIT 2003
`Azurity Pharmaceuticals, Inc. v. Helsinn Healthcare S.A.
`IPR2025-00945
`Page 1 of 10
`Number of times this article has been viewed
`This article was published in the following Dove Press journal:
`Therapeutics and Clinical Risk Management
`8 May 2009
`This article was published in the following Dove Press journal:
`Therapeutics and Clinical Risk Management
`8 May 2009
`This article was published in the following Dove Press journal:
`Therapeutics and Clinical Risk Management
`8 May 2009
`
`
`
`
`
`
`
`Therapeutics and Clinical Risk Management 2009:5376
`Ruhlmann and Herrstedt Dovepress
`submit your manuscript | www.dovepress.com
`Dovepress
`became commercially available. The second drug in this
`class, casopitant (casopitant mesylate), has now completed
`phase II and phase III trials, demonstrating efficacy in
`the same magnitude as demonstrated with aprepitant.
`Previous indications for casopitant, overactive bladder, social
`anxiety disorder, major depressive disorder, insomnia, and
`fibromyalgia have been revoked, and remaining indications
`are CINV and postoperative nausea and vomiting (PONV).
`This review delineates the properties and clinical use of
`casopitant in the prevention of chemotherapy-induced nausea
`and vomiting. It should be noted, that most of the clinical
`data is availably in abstract form only.
`Neuropharmacology of emesis
`Insight in the complex human emetic pathway has been
`achieved primarily on the basis of animal models.
`10 It is a
`general assumption, that the vomiting centre (VC) in the
`medulla oblongata, the chemoreceptor trigger zone (CTZ)
`in the area postrema (AP) on the caudal margin of the IVth
`ventricle, the visceral afferent neurons and abdominal vagal
`afferent neurons, form the central emetic pathway.
`11 The
`VC is representing anatomical structures at the level of the
`nucleus tractus solitarius (NTS) and the visceral and somatic
`motor nuclei. Another acceptation is that CINV results from
`directly activation of the NTS by visceral afferent neurons
`and/or by inputs from the CTZ. The CTZ, in turn, may
`be stimulated by abdominal vagal afferent activation by
`release of serotonin (5-HT
`3) from the enterochromaffin cells
`(EC cells) in the gut. The reflex activation of the NTS and the
`CTZ further extends to the visceral and somatic motor nuclei
`giving rise to physiological changes, resulting in nausea and
`vomiting.
`12 Radioligand binding studies have identified the
`binding affinity of several neurotransmitters to receptors
`such as dopamine (D
`2), muscarine cholinergic, histamine
`(H1) and serotonin (5-HT3), involved in the emetic response
`to chemotherapy.10 The fundamental role for serotonin and
`5-HT3
`_receptors in the emetic pathway was discovered in
`the mid 1980s, giving rise to the development of 5-HT 3-
`receptor antagonists.13 Recently, the role of substance P and
`the neurokinin1 (NK1) receptors in the emetic pathway has
`been investigated, resulting in development of the NK 1
`receptor antagonists.
`Substance P and NK1 receptor
`antagonists
`Substance P (SP) was isolated in 1931 but not purified and
`sequenced until 1970.
`14,15 SP is a member of a family of small
`peptides, the mammalian tackykinins (TKs).16 Three receptors
`for TKs (NK 1, NK2, and NK 3) have been cloned, with SP
`being the preferred agonist at NK 1 receptors. 16 The role
`of SP in emesis dates back to 1984, when Carpenter and
`colleauges demonstrated that systemic administration of
`the neuropeptide caused emesis in dogs.
`17 In 1993, Andrews
`and Bhandari suggested that resinferatoxin exerts its potent
`antiemetic activity by depleting SP at a central site in the
`emetic pathway, possibly in the NTS.
`18 Penetration of the
`blood-brain barrier is essential for the antiemetic activity
`of systemically administered NK
`1 receptor antagonists, a
`quality that the peptide-based NK1 receptor antagonists did
`not exhibit.19,20 Hence a milestone was reached, when the first
`nonpeptide NK1 receptor antagonist, CP-96,345, with high
`affinity for the NK1 receptor, was developed in 1991.21 This
`finding was followed by a number of experimental studies
`confirming a broad-spectrum antiemetic activity of non-
`peptide NK
`1 receptor antagonists. 22–25 These studies led to
`the development of the latest class of antiemetic agents, with
`aprepitant being the first clinically available NK
`1 receptor
`antagonist. Casopitant has now completed phase III trials
`for the prevention of CINV from moderately and highly
`emetogenic chemotherapy.
`Metabolism, pharmacokinetics,
`and interactions
`Preclinical studies
`Only sparse information about the ADME (absorption,
`distribution, metabolism, and excretion) properties of caso-
`pitant (oral and intravenous formulation) has been published.
`Casopitant is a piperazine derivative [1-piperidinecarboxamide,
`4-(4-acetyl-1-piperazinyl)-N-((1R)-1(3,5-bis(trifluorometh
`yl)phenyl)-ethyl)-2-(4-fluoro-2-methylphenyl- N-methyl-
`(2R,4S)-; GW679769] (Figure 1).
`26 In a ferret-model of cis-
`platin-induced emesis, GW679769 (casopitant) inhibited
`retching and vomiting and reduced nausea-like behaviours
`in a dose-dependent manner.
`27–29 Several clinical trials have
`assessed safety, potential interactions and pharmacokinetic
`properties of casopitant; however many data is available in
`abstract form only.
`The pharmacokinetics and brain penetration of casopi-
`tant were studied in the ferret-model of cisplatin-induced
`emesis. Following a single intraperitoneal dose, radioactive
`labeled casopitant ([
`14C] casopitant) was rapidly absorbed,
`with plasma and brain concentrations being approximately
`equal at two hours post-dosing. [
`14C] casopitant was found
`in the brain as the parent compound and two major oxidative
`metabolites (M1 and M2), accounting for approximately
`Page 2 of 10
`
`
`
`
`
`
`
`Therapeutics and Clinical Risk Management 2009:5 377
`Casopitant in chemotherapy-induced nausea and vomitingDovepress
`submit your manuscript | www.dovepress.com
`Dovepress
`76%, 19%, and 3% of the radioactivity, respectively;
`suggesting that the pharmacologic activity of casopitant in
`the ferret is largely attributable to the parent compound.
`26
`An in vitro receptor binding affinity study describes, that
`casopitant possesses a high affinity for brain NK1 receptors
`in the ferret.26
`Because casopitant is intended to be administered in
`combination with a 5-HT3-receptor antagonist and because
`therapeutic synergy has been observed with this combina-
`tion in the ferret, a drug interaction study was conducted.
`28
`Following co-administration of ondansetron and casopitant
`in ferrets, no alteration of disposition of either agent was
`seen. A synergistic antiemetic activity was demonstrated,
`proposing complementary mechanisms of pharmacologic
`actions of the two agents.
`30 No information about animal
`toxicity was described in the studies above.
`Clinical studies
`Pharmacokinetic and pharmacodynamic aspects (PK/PD)
`of casopitant were assessed in two phase II trials (2802 PK
`samples from 765 subjects) in patients undergoing treatment
`with moderately and highly emetogenic chemotherapy (MEC
`and HEC). In addition to ondansetron and dexamethasone,
`patients received placebo; 50-, 100-, or 150 mg daily of oral
`casopitant
`for three days; or a single oral dose of 150 mg
`casopitant, starting prior to chemotherapy on day 1. The dis-
`tribution of casopitant follows a two-compartment first-order
`model, and the oral absorption was in general rapid, however
`30% of subjects exhibited delayed and slow oral absorp-
`tion. Oral clearance was 17.4 L/h/70 kg, displaying a large
`intersubject variability (72%). Body weight was identified
`as a significant covariate of casopitant clearance and central
`volume of distribution. Further, it was shown that low
`casopitant area under the curve (AUC) in patients receiving
`HEC increased the risk of emesis in some patients, suggesting
`that high concentrations of casopitant during the first 24 h
`may be important for adequate pharmacological response.
`Oral casopitant administered as a single dose of 150 mg on
`day 1, or followed by 50 mg doses on days 2 and 3, seem
`to provide adequate receptor occupancy and prevention of
`CINV associated with MEC and HEC.
`31
`A PK/PD study analyzed data (1637 PK samples from
`562 subjects) from a phase II trial in which casopitant was
`evaluated for the prevention of PONV. Patients were female
`and undergoing surgery and at high risk for PONV. In addi-
`tion to ondansetron, patients received placebo; 50, 100, or
`150 mg single oral doses of casopitant prior to surgery. In
`this study oral clearance was 24.4 L/h/70kg, displaying
`moderate intersubject variability (48%). Body-weight was
`also identified as a significant covariate of casopitant central
`volume of distribution, but not of clearance. For the treatment
`of PONV in high-risk patients, a dose of 50 mg casopitant is
`suggested to be the minimally effective dose.
`32
`Casopitant is a substrate and weak-to-moderate
`inhibitor of CYP3A4. 33 Based on the role of CYP3A4 in
`the metabolism of several antiemetic drugs, pharmaco-
`kinetic interactions between casopitant, dexamethasone
`(substrate and inducer of CYP3A4) and ondansetron (mixed
`CYP substrate) were assessed in a two-part, three-period,
`single-sequence phase I study in 44 healthy adult subjects.
`The study aimed at investigating possible changes in bio-
`availability of casopitant, ondansetron and dexamethasone,
`when these agents are co-administered. In Part 1, which was
`representative of a three-day regimen for the prevention of
`CINV resulting from HEC, subjects received oral casopi-
`t
`ant (150 mg, day 1; 50 mg, days 2–3) in regimen A; oral
`dexamethasone (20 mg, day 1; 8 mg twice daily, days 2–3)
`and IV ondansetron (32 mg, day 1) in regimen B; and oral
`casopitant (150 mg, day 1; 50 mg, days 2–3), a reduced
`d
`ose of oral dexamethasone (12 mg, day 1; 8 mg once daily,
`days 2–3), and IV ondansetron (32 mg, day 1) in regimen C.
`In Part 2, which was representative of a three-day regimen
`for the prevention of CINV resulting from MEC, subjects
`received oral casopitant (150 mg, day 1; 50 mg, days 2–3) in
`r
`egimen D; IV dexamethasone (8 mg, day 1; 8 mg twice daily,
`days 2–3) and oral ondansetron (8 mg twice daily, day 1)
`i
`n regimen E; and oral casopitant (150 mg, day 1; 50 mg,
`days 2–3), IV dexamethasone (8 mg, day 1; 8 mg twice daily,
`days 2–3), and oral ondansetron (8 mg twice daily, day 1)
`Casopitant
`O
`O
`N
`N
`N
`F
`F F
`F
`F
`F
`F
`N
`Figure 1 Structure of casopitant.
`Page 3 of 10
`
`
`
`
`
`
`
`Therapeutics and Clinical Risk Management 2009:5378
`Ruhlmann and Herrstedt Dovepress
`submit your manuscript | www.dovepress.com
`Dovepress
`in regimen F. Blood samples for PK analysis were collected
`at fixed times. The pharmacokinetic results of the Part 2
`regimens demonstrated a 28% increase in mean casopitant
`AUC on day 1, when casopitant was co-administered with
`12 mg oral dexamethasone and 32 mg ondansetron compared
`to casopitant administered alone. Further, it was shown that
`on Day 1, the lower dose of dexamethasone (12 mg) as
`used in regimen C resulted in a lower mean dexamethasone
`AUC and maximum concentration (C
`max), by 17% and 35%,
`respectively, when compared to dose regimen B (20 mg
`of dexamethasone). Dose normalization of the pharmaco-
`kinetic parameters showed that casopitant increased the
`AUC of oral dexamethasone by 39%. After three days of
`co-administration, AUC resulting from 8 mg once daily of
`oral
`dexamethasone combined with 50 mg oral casopitant
`was similar to that resulting from 8 mg twice daily of oral
`dexamethasone alone. Plasma exposures of 32 mg ondanse-
`tron were not affected by co-administration with casopitant.
`The results of Part 2 showed a 16% increase in mean caso-
`pitant AUC on day 1, when casopitant was co-administered
`with
`8 mg oral dexamethasone and 8 mg ondansetron twice
`daily, compared to casopitant administered alone. As to dexa-
`methasone an increase in AUC day 1 by 21% was observed
`when dexamethasone (8 mg) was co-administrered with
`150 mg casopitant and 8 mg ondansetron twice daily. The
`pharmacokinetics of ondansetron in Part 2 was not altered
`by co-administration with casopitant. All dose regimens
`were generally well tolerated, with headache and dizziness
`being the most commonly reported adverse events (AEs). In
`conclusion, the study suggests a reduction in dexamethasone
`dose of 40%–50%, when repeat-dose oral dexamethasone is
`to be co-administered with oral casopitant, whereas there is
`no need to change the dose of ondansetron or casopitant.
`34
`In another phase I, two-part, two-period study, the effect
`of casopitant on the pharmacokinetics of two 5-HT 3-RAs,
`dolasetron and granisetron, was investigated. Dolasetron
`is reduced to its active metabolite, hydrodolasetron, which
`is metabolized by CYP2D6 with minor involvement of
`CYP3A4. Plasma exposures of hydro-dolasetron are usually
`increased approximately threefold in CYP2D6 poor metabo-
`lizers (PMs) as compared to extensive metabolizers (EMs).
`For CYP2D6 PMs, CYP3A4 is likely to play a larger role in
`the clearance of hydrodolasetron, and these subjects may be
`more sensitive to co-administration of inhibitors of CYP3A4,
`such as casopitant. Granisetron is primarily metabolized
`by CYP3A4 with a minor contribution from CYP1A1. A total
`of 18 subjects, (nine were CYP2D6 EMs and nine were
`CYP2D6
`PMs), received oral dolasetron 100 mg days 1–3
`(period 1), and 5–14 days later the same dose of dolasetron
`combined with oral casopitant 150 mg day 1, and 50 mg days
`2–3 (period 2). The granisetron cohort (19 subjects) received
`oral granisetron 2 mg days 1–3 (period 1), and 5–14 days
`later combined with oral casopitant 150 mg day 1, and 50 mg
`days 2–3 (period 2). Blood samples for PK analysis were
`collected at fixed times. The largest changes in hydrodolas-
`etron exposure after coadministration with casopitant were
`seen in CYP2D6 EMs, with a 24% increase in hydrodolas-
`etron AUC on day 1 and 30% increase in C
`max on days 1 and 3.
`All other changes in hydrodolasetron exposure were 20%,
`and granisetron exposure was not altered to any relevant
`extent (11%). None of the changes observed are considered
`clinically meaningful. Coadministration of casopitant with
`dolasetron or granisetron was well tolerated.
`33
`In a phase I trial, the effect of casopitant on the PK and PD
`of steady-state warfarin in healthy adults was studied. I n vitro
`studies had shown that casopitant is a dose and duration-
`dependent inhibitor of CYP3A4, and a moderate inducer of
`CYP2C9. These enzymes are important in the metabolism of
`warfarin. Subjects received warfarin and were randomized
`to
`receive either casopitant, 150 mg day 1, 50 mg days 2 and
`3, and warfarin, days 1–10, or casopitant, 60 mg daily, and
`warfarin, days 1–14. When casopitant was administered for
`three days, there was no significant alteration in steady-state
`C
`max and AUC of R- and S-warfarin. In the other regimen
`R- and S-warfarin AUC was increased 1.31- and 1.27-fold,
`respectively. However, steady-state international normal-
`ized ratio (INR) was not significantly affected with either
`regimen.
`35
`A number of other studies have addressed the role of
`CYP-enzymes and drug-interactions with casopitant. These
`studies enrolled a limited number of patients, but it seems
`likely that casopitant can be administered safely with drugs
`metabolized by CYP3A4, such as cyclophosphamide and
`docetaxel.
`36,37 Vinorelbine and etoposide, (likely to be
`co-administered with cisplatin), are metabolized by CYP3A,
`potentially leading to increased plasma levels of these agents
`when co-administered with casopitant. Oral contraceptives
`are also metabolized by CYP3A-enzymes. Co-administration
`of casopitant and oral contraceptives may result in lower
`levels of the hormones, causing the oral contraceptives to be
`an uncertain method of contraception when co-administred
`with casopitant. No data on these potential interaction risks
`have been published.
`Ketoconazole is a strong CYP3A4 inhibitor. A phase I
`study characterized the effect of ketoconazole on the PK
`of casopitant, demonstrating a four- to six-fold increase
`Page 4 of 10
`
`
`
`
`
`
`
`Therapeutics and Clinical Risk Management 2009:5 379
`Casopitant in chemotherapy-induced nausea and vomitingDovepress
`submit your manuscript | www.dovepress.com
`Dovepress
`in casopitant exposure. However no safety concerns were
`noted.38 Y et another phase I study was conducted to investi-
`gate the potential of casopitant to prolong the QTc interval
`in supratherapeutic doses and when combined with keto-
`conazole. Compared with placebo, no significant impact on
`QTc was observed.
`39
`No available data has been published as concerns; oral
`absorption fraction, influence of concomitant food consump-
`tion, half-life, or percentage of NK
`1 receptor occupancy
`needed for optimal efficacy of casopitant.
`Clinical development
`The clinical development of casopitant in preventing CINV
`comprises phase I, phase II, and phase III trials. In the section
`above phase I trials were described. Phase II and phase III
`trials handle documentation for casopitant in the prevention
`of CINV in patients receiving MEC and HEC, respectively.
`Phase ii trials
`Patients treated with MeC
`A large phase II, multicenter, randomized, double-blind,
`placebo-controlled, dose-ranging, parallel group trial,
`evaluated the addition of casopitant to standard prophy-
`laxis (ondansetron plus dexamethasone) in patients receiv-
`ing MEC.
`40 Primary endpoints were rates of complete
`response (CR), defined as no vomiting or retching, no
`use of rescue antiemetics and no premature withdrawal
`during the first 120 hours after initiation of MEC; and no
`significant nausea (SN), during the first 120 hours after
`initiation of MEC. The MEC regimens used were: cyclo-
`phosphamide (500–1500 mg/m
`2) with another unspecified
`MEC; cyclophosphamide (750–1500 mg/m 2) alone; oxali-
`platin (85 mg/m2); doxorubicin (60 mg/m2); epirubicin
`(90 mg/m2); or carboplatin AUC 5. Patients were strati-
`fied by gender and taxane use. 719 patients were randomized
`to six arms; arms 5 and 6 being exploratory. In addition to
`ondansetron 8 mg twice-daily day 1–3 and dexamethasone
`8 mg IV day 1, Patients in arms 1–5 received either placebo,
`casopitant 50 mg daily days 1–3, casopitant 100 mg daily days
`1–3, casopitant 150 mg daily days 1–3, or casopitant 150 mg
`day 1. Patients in arm 6 received ondansetron 16 mg daily
`days 1–3, dexamethasone 8 mg day 1 and casopitant 150 mg
`daily days 1–3. CR (120 h) was achieved in 81% of patients
`receiving 50 mg casopitant, compared to 70% in the control
`arm (p = 0.0410). CR (120 h) rates for the 100 mg and 150 mg
`casopitant arms were 79% and 85%, respectively (p = 0.1092,
`0.0124). There were no significant differences among groups
`in the rates of CR (24 h) or no SN. The exploratory arm 5,
`casopitant 150 mg day 1, was of particular interest, with CR
`(120 h) rate and no SN rate of 80% and 66%, respectively,
`in arm 6 the figures were 84% and 70%. The antiemetic
`r
`egimens were well tolerated, with nausea, fatigue and neutro-
`penia being the most common side effects.40
`A subgroup analysis from the phase II trial examined the
`antiemetic efficacy in patients (n = 124) with gastrointestinal
`cancers receiving oxaliplatin 85 mg/m2. The majority were
`diagnosed with colorectal cancer (90%). CR was achieved
`in 83%, 76%, and 86% in the three casopitant arms (50 mg,
`100 mg, and 150 mg, respectively), compared to 61% in the
`control arm. Although one should be cautious with interpre-
`tation of data of a small subgroup analysis, CR rates were
`similar with those of the complete dataset.
`41
`Safety and efficacy of casopitant in women with breast
`cancer, was considered in another subgroup analysis
`of the phase II trial. Patients (n = 176) received one or
`more of the following regimens: cyclophosphamide (C)
`(500–1500 mg/m
`2) with another unspecified MEC; cyclo-
`phosphamide (750–1500 mg/m 2) alone or with another
`minimally emetogenic agent; doxorubicin (A) (60 mg/m2);
`or epirubicin (E) ( 90 mg/m 2). The majority received a
`combination of AC or EC (n = 102) or a taxane (n = 37).
`This subgroup analysis found that CR rates were similar
`to the overall response profile. The antiemetic regimens
`were generally well tolerated. Nausea (24%), alopecia
`(17%), neutropenia (16%), anorexia (13%), and fatigue
`(12%), were the most commonly reported side effects in
`this patient group.
`42
`Patients treated with HeC
`Another phase II trial examined the antiemetic efficacy of
`casopitant in addition to standard antiemetic prophylaxis
`in patients receiving cisplatin (70 mg/m
`2) day 1.43 It was
`conducted as a multicenter, randomized, double-blind,
`placebo-controlled, dose-ranging, parallel group study.
`Patients (n = 493) were stratified by gender and randomized
`a
`mong six arms. All patients received ondansetron 32 mg
`IV day 1 and dexamethasone PO day 1–4. The casopitant
`doses in arms 2, 3, and 4 were the same as in the phase II, MEC
`s
`tudy (50 mg, 100 mg, and 150 mg daily days 1–3) and com-
`pared to placebo in arm 1. Arms 5 and 6 were exploratory with
`c
`asopitant 150 mg day 1 and aprepitant (125 mg day 1 and
`80 mg day 2–3), respectively. As in the MEC study, results
`demonstrated that casopitant significantly improved the CR
`(
`120 h) rates. CR (120 h) was achieved in 76% of patients
`receiving 50 mg casopitant compared to 60% in the control
`arm. CR (120 h) rates for the 100 mg and 150 mg casopitant
`Page 5 of 10
`
`
`
`
`
`
`
`Therapeutics and Clinical Risk Management 2009:5380
`Ruhlmann and Herrstedt Dovepress
`submit your manuscript | www.dovepress.com
`Dovepress
`arms were 86% and 77%, respectively. Again it was revealed
`that casopitant administered as a single dose, 150 mg day 1,
`resulted in a similar high response rate, 75%. The CR (120 h)
`was 72% for the three-day aprepitant regimen. The preven-
`tion of emesis in the 24 hours after cisplatin was similar in
`all groups with CR rates in the range of 86%–96%. Again
`the addition of casopitant to standard prophylaxis was well
`tolerated. Neutropenia, nausea and hiccups ( 17%) were
`the most common side effects reported.
`43
`The phase II studies indicated that a single dose of
`casopitant 150 mg was as good as a three-day regimen. Further-
`more no evident dose-efficacy correlation was observed
`(although casopitant 50 mg and 150 mg was superior to
`casopitant 100 mg in the phase II MEC trail, as the latter was
`insignificant). Emergence of the intravenous formulation of
`casopitant and the results from the phase II trials contributed
`to the design of the phase III trials.
`Phase iii trials
`Patients treated with MeC
`The phase III, MEC study was a multinational, double-blind,
`placebo-controlled trial.
`44,45 Patients (n = 1933, 95% diagnosed
`with breast cancer) received a regimen consisting of an
`anthracycline plus cyclophosphamide (AC). In addition to
`a
`ntiemetics in the control arm (dexamethasone 8 mg IV day 1
`and ondansetron 8 mg twice daily PO day 1–3) patients were
`randomized to receive either placebo (control) or one of three
`dosing regimens: casopitant 150 mg PO day 1; casopitant
`150 mg PO day 1 and 50 mg PO day 2–3; or casopitant
`90
` mg IV day 1 and 50 mg PO day 2–3 (Table 1). Therapy
`was continued for up to four cycles. The primary endpoint
`was CR rate (120 h), defined as no vomiting or retching,
`no use of rescue antiemetics and no premature withdrawal
`during the first 120 hours after initiation of chemotherapy. All
`casopitant arms were superior to the control arm as concerns
`CR rates. In the group of patients receiving the single oral
`dose of casopitant, CR (120 h) was 73% as compared to 59%
`in controls (p 0.0001 for all treatment arms) in the first
`treatment cycle (Figure 1), and the improvement appeared
`to be maintained through cycles two to four. An improve-
`ment was also demonstrated for the secondary endpoint,
`no vomiting. Similar observations were noticed for the
`group receiving casopitant 150 mg PO day 1 and 50 mg PO
`day 2–3, with CR (120 h) at 73%.
`44 Finally, patients in the
`T able 1 Dose regimens, complete response (CR), and no emesis (ee) of phase ii and phase iii clinical trials in patients receiving MeC
`or HeC
`Clinical trial Study arm CR (120) No EE (120)
`Phase ii, MeC Control regimen: Ond 8 mg bid D1–3 + Dex 8 mg iv D1 70% NA
`Cas 50 mg D1–3 + Control regimen 81% NA
`Cas 100 mg D1–3 + Control regimen 79% NA
`Cas 150 mg D1–3 + Control regimen 85% NA
`Cas 150 mg D1 + Control regimen 80% NA
`Cas 150 mg D1–3 + Ond 16 mg D1–3 + Dex 8 mg iv D1 84% NA
`Phase
`ii, HeC Control regimen: Ond 32 mg iv D1 + Dex D1–4 60% NA
`Cas 50 mg D1–3 + Control regimen 76% NA
`Cas 100 mg D1–3 + Control regimen 86% NA
`Cas 150 mg D1–3 + Control regimen 77% NA
`Cas 150 mg D1 + Controll regimen 75% NA
`Aprep 125 mg D1, 80 mg D2–3 + Control regimen 72% NA
`Phase
`iii, MeC Control regimen: Ond 8 mg bid D1–3 + Dex 8 mg iv D1 59% 63%
`Cas 150 mg D1 + Control regimen 73% 80%
`Cas 150 mg D1, Cas 50 mg D2–3 + Control regimen 73% 81%
`Cas 90 mg
`iv D1, Cas 50 mg D2–3 + Control regimen 74% 78%
`Phase
`iii, HeC Control regimen: Ond 32 mg iv D1 + Dex 20 mg D1, Dex 8 mg bid D2–4 66% 68%
`Cas 150 mg D1 + Control regimen* 86% 89%
` Cas 90 mg iv D1, Cas 50 mg D2–3 + Control regimen** 80% 83%
`Notes: *Ond 32 mg iv D1 + Dex 12 mg D1, Dex 8 mg bid D2-4; **Ond 32 mg iv D1 + Dex 12 mg D1, Dex 8 mg D2–4.
`Abbreviations: A prep, aprepitant; CR, no emesis and no need for rescue antiemetics for 0–120 hours; bid, twice daily; Cas, casopitant; D, day(s); Dex, dexamethasone; HeC, highly
`emetogenic chemotherapy; iv, intravenous; MeC, moderately emetogenic chemotherapy; NA, not available; No ee, no emetic episodes for 0–120 hours; Ond, ondansetron.
`Page 6 of 10
`
`
`
`
`
`
`
`Therapeutics and Clinical Risk Management 2009:5 381
`Casopitant in chemotherapy-induced nausea and vomitingDovepress
`submit your manuscript | www.dovepress.com
`Dovepress
`IV/PO group experienced improvement of emesis over the
`first 120 hours after MEC. CR (120) was increased to 74%
`versus 59% in the control group, and again improvement
`was maintained in repeat cycles of MEC.
`45 No significant
`differences in protection from nausea was seen. There were
`no differences in distribution and occurrence of side effects
`among the groups. Neutropenia (with sequelae at 3% inci-
`dence were seen in all arms), alopecia, fatigue, leukopenia
`and constipation were the most commonly experienced side-
`effects; there were only few reports of injection site reactions,
`and these were seen slightly more frequently in the IV/oral
`group.
`44,45 It is noteworthy that casopitant administered as
`a single oral dose exhibits similar efficacy as the three-day
`IV/oral dose regimen.
`Patients treated with HeC
`The phase III, HEC trial was conducted to assess the impact
`of casopitant, when used in combination with ondansetron
`and dexamethasone as compared to ondansetron and dexa-
`methasone alone.
`46,47 810 patients received cisplatin-based
`chemotherapy in a dose of 70 mg/m 2 and participated
`in a maximum of six cycles. The study was designed as
`multinational, double-blind and placebo-controlled. The
`control regimen consisted of ondansetron 32 mg IV plus
`dexamethasone 20 mg PO day 1, and dexamethasone 8 mg
`PO twice daily day 2–4 (Table 2). Patients were randomized
`to the control regimen or one of two experimental arms: a
`single dose of casopitant 150 mg PO; a three-day IV/oral
`dose, consisting of casopitant 90 mg IV day 1 and casopitant
`50 mg PO day 2–3. The primary endpoint was complete
`response in the first 120 hours (CR, 120 h) after initiation
`of HEC. In the casopitant 150 mg PO day 1 arm a statisti-
`cally significant increase of 20% (86% vs 66% in controls,
`p = 0.0001) in the number of patients with CR (120 h) was
`obtained (Figure 2), and this was maintained over multiple
`cycles. For the HEC regimen casopitant also demonstrated
`efficacy with regard to several secondary endpoints: CR
`(24 h) rates were 95% and 88% for the casopitant 150 mg
`and control groups, respectively (p = 0.0044); and interest-
`ingly improvements in no significant nausea (no SN), no
`nausea (NN) and no vomiting (NV) for both the acute and
`delayed phases, were observed as well.
`46 Casopitant given
`as a three-day IV/oral dose regimen also demonstrated to be
`superior to the control arm. CR (120 h) was achieved in 80%
`of patients (p = 0.0004) and CR (24 h) was 94% in this group
`(p = 0.0165), moreover efficacy was maintained over multiple
`cycles. Again clinically meaningful improvements were
`observed for no SN, NN, or NV.
`47 Casopitant was generally
`well tolerated. The most frequently reported side effects were
`neutropenia, leukopenia and anemia occurring with similar
`frequency in the experimental- and control arms.
`46,47
`Quality of life
`Using the Functional Living Index – Emesis (FLIE) ques-
`tionnaire,
`